Diastasis Recti: 6 Top Tips for Early Healing
Diastasis recti at the end of pregnancy is normal, and the majority will resolve in the early weeks postnatal. Follow these 6 top tips to set yourself up for success in healing your diastasis recti in the fourth trimester.
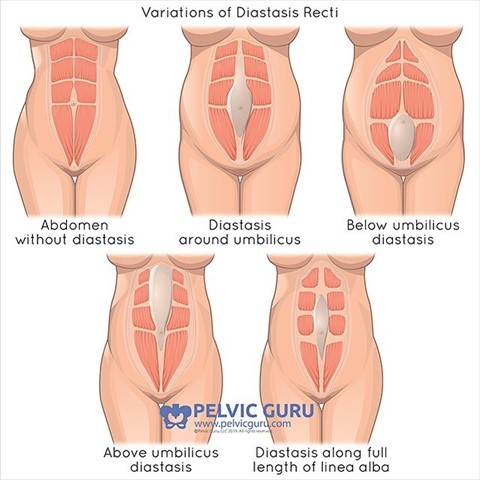
Diastasis recti is thinning and widening of the linea alba (the connective tissue in the midline abdominal wall between the 2 sit-up muscles) with associated laxity of the abdominal wall. You will often hear it called “tummy muscle separation” or “mummy tummy” due to its characteristic pendular appearance.
The term “separation” is misleading and probably leaves you feeling totally depressed about your tummy muscles. If no hernia is present (which is most women with diastasis recti) nothing has separated. Great news, but if nothing truly separates what is going on?
The linea alba thins and stretches, increasing space between the 2 sit-up muscles, creating the “gap”. This must occur to accommodate the growing baby during pregnancy.
Think of a guy with a 6-pack. There is always a space between the 2 sit-up muscles, but pregnancy increases this, and you will notice a reduction in tension along the tummy.
As frustrating as diastasis recti can be, it does not cause harm or significant risk to your health (well your physical health anyway). We know that diastasis recti has been correlated with negative body image and lower self-confidence; however, research has demonstrated no link between diastasis recti and pelvic floor dysfunction, or pelvic organ prolapse.
How to recognise a diastasis Recti
Typically, you will see bulging or doming of the midline of the tummy on getting up and down from lying or lifting something. Or I often hear women complain of feeling that they look like they are still pregnant.
Currently, the “Rec Check” is used to identify diastasis recti. At The Bump Room we have created a Diastasis Recti eBook available for free download on the free resources section on the website www.thebumproom.ie/free-resources/. A detailed description of the “Rec Check” is in this eBook.

What is normal?
Slight separation towards the end of pregnancy should be considered a normal and necessary adaptation for the growing baby. A study by da Mota and colleagues (2015) found that 100% of women had diastasis recti by gestational week 35. The prevalence decreased to 52.4% at 4-6 weeks postnatal and continued to decrease to 39% at 6 months. So, you are not alone.
For the majority, a diastasis recti resolves naturally in the weeks after childbirth. Natural healing occurs in the first 8 weeks after the baby is born. Follow these top tips for helping your body heal your diastasis recti early.
6 Top Tips To Promote Healing
1. Avoid constipation/straining
Constipation will put excess pressure on your diastasis recti if you strain or bear down while going to the bathroom because it creates bulging pressure in both the pelvic floor and the abdominal wall. This puts unhealthy stress on your diastasis.
To reduce the bulging pressure, you might benefit from making some simple adjustments to your bathroom habits. While sitting on the toilet, elevate your feet on a footstool to optimise the shape of the rectum and reduce straining. Leaning forward can also help. Think of a man reading the paper while on the toilet!! Men also take their time on the toilet whereas women tend to rush in and out which does not help the pelvic floor relax to allow an easy bowel motion.
Fluid intake is important in avoiding constipation. Remember if you are breastfeeding increase your fluids to support the increased fluid demands. Getting a re-useable water bottle with markings on it can be a great reminder (it’s hard for baby brain to remember everything).
Fill up on fibre. It’ll make your stool softer and easier to pass. Opt for whole grains, fruits, vegetables, and legumes as much as possible, and limit your intake of bowel cloggers like white bread, pasta, or rice. This is a job to outsource to your partner or family member. Having fibre-rich healthy snacks readily available meant that you don’t grab sugary low fiber food between baby feeds.
Get moving. No one’s expecting you to run laps, of course. But try to get up and start taking short walks. Too much time sitting or lying down can cause a backup.
If all this fails ask your GP about a stool softener. If you’re still having trouble, stool softeners, laxatives and, in some cases, suppositories can help you get going.
2. Avoid movements that cause doming
In the first 8 weeks postnatal, you want to do your best not to put too much stress on your diastasis. It is best to minimise movements that create repeated doming of the diastasis recti. Sometimes these might be simple everyday movements like sitting up in bed or lifting something heavy.
You may be best rolling to the side to get up rather than the traditional sit-up action. Minimising lifting (as best possible) can also minimise the pressure on the recovering diastasis recti.
Remember this is just for the early weeks as soon as doming resolves it is perfect to get back to getting out of bed without thinking about how you are doing it. A little doming every now and again will not harm your diastasis but repetitive doming created unnecessary stress on your recovering diastasis.
3. Tummy Support
Abdominal supports are recommended for women who struggle to control the doming of their diastasis recti in the first few weeks postnatal.
The physiotherapist on the postnatal ward may have provided you with a Tubigrip in a size K or L to support the diastasis if it is greater than 3 fingers or is quite deep. If you don’t mind wearing this support it is a great option and there may not be any need to purchase anything else.
Another great option is the SRC Recovery Shorts and Leggings. These have Anatomical Support Panels, and the top front panel supports the upper and lower abdomen decreasing inter rectus distance and helping promote healing. More information is available at http://srchealth.com/products/src-recovery-shorts.
Use the code: THEBUMPROOM for 10% off any purchase.

Tummy support will bring the 2 sits of the sit-up muscle closer together which makes sense in the first 8 weeks after birth to encourage this natural healing. After this period it is time to wear off the supports as exercise is the key to restoring your tummy muscle function after this period.
4. Diet and nutrition
Healing tissue requires the necessary vitamins and minerals to carry out the repair.
Foods high in vitamins C, E, and A are essential when it comes to recovering from diastasis recti. These vitamins aid in collagen production and promote the healing of connective tissue. They can be found in colorful, delicious fruits and veggies including oranges, kiwis, strawberries, pineapple, dark leafy greens, red peppers, tomatoes, avocados, asparagus, sweet potatoes, carrots, and broccoli.
Protein is vital for repairing tissue so aim to include some protein with every meal.
Zinc is essential to connective tissue production and can be found in lentils, pumpkin and sesame seeds, sardines, tofu, red meat, poultry, oysters, and mushrooms.
You will probably notice that after a large meal or eating food that cause bloating your diastasis may feel worse. Let me reassure you that it is not worse it is just that your tummy muscles can’t provide as much resistance as they used to so bloating will appear worse. Avoiding food that cause bloating for you will help you feel better in yourself.
5. Breathing
There is a unique relationship and synergy between the diaphragm, abdominal wall, and pelvic floor. This can be compromised in pregnancy as your baby grows. Your tummy muscles get lengthened, and your diaphragm gets squished up (remember the shortness of breath on the stairs).
As your body learns new ways of functioning with diastasis recti including altered breathing strategies might be your body’s way of compensating for the lack of tension and strength in the tummy muscles.
This may include breath-holding during strenuous tasks (picking up your baby), getting out of the chair or exercising, leading to increased intraabdominal pressure and excessive strain on the midline connective tissue.
I see a lot of postnatal women who tend to “grip” or “overuse” their upper abdominal muscles which restricts breathing. Overusing the upper abdominal muscles will push out the lower tummy and make the diastasis appear more pronounced.
Try noticing if you are holding your breathing during the day. Practice letting go of any gripping in your tummy muscles, breathing gently in and out so that the belly rises on a breath in and falls on a breath out.
You can find out more about breathing in our diastasis eBook Diastasis Recti eBook
6. Gentle tummy tensioning exercises
The leaflet from the postnatal ward is likely to include basic core exercises to help generate tension in the diastasis recti. These are great for the first 2-4 weeks after birth. I would encourage you to do these exercises regularly to help stimulate healing.
As these exercises become easy you will need to increase the challenge as your body is able. Download out FREE Diastasis eBook here to find out some more great diastasis recti exercises Diastasis Recti eBook.
After 8 weeks
No improvements are seen after 8 weeks postnatal unless you are exercising and loading the linea alba appropriately. Abdominal load refers to the difficulty and effort of exercise applied to the abdominal wall.
Getting the right level of load is about being able to carry out an exercise without excessive doming or lack of tension. This is best done with the support of a physiotherapist specialising in women’s health as underloading the abdominal wall with exercises that are too easy is unlikely the make the desired changes.
Check out our online LIVE postnatal classes available when you join The Bump Room Community. Here you can exercise under the guidance of a chartered physiotherapist who specialises in women’s health from the comfort of you own home. Find out more HERE.
Diastasis recti is a source of significant stress and anxiety for postnatal women. While most resolve in the first 8 weeks some women still have diastasis recti at 6 months postnatal. The body can always adapt so it is never too late for women to start a rehabilitation programme, however, it is best managed in the early postnatal phase.
